Multiple sclerosis (MS) is widely understood as an autoimmune disorder where the body attacks the protective myelin sheath surrounding nerve fibers. However, a groundbreaking study published in Nature reveals a deeper, more insidious mechanism driving the disease’s most debilitating phase: the death of specific brain cells that underpin human cognition.
Researchers have identified why certain neurons are uniquely vulnerable to MS, uncovering a biological flaw that may explain why current treatments fail to stop cognitive decline and brain shrinkage in progressive stages of the disease.
The Hidden Cost of Being Human
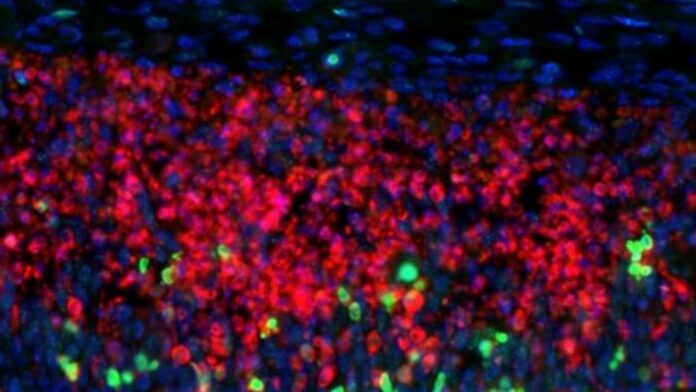
The study focuses on a specific group of neurons known as CUX2 cells, located in the outermost layer of the brain’s cortex. These cells are critical for complex cognitive functions, such as reasoning and memory processing—traits that distinguish human intelligence from that of other mammals.
While these cells are essential for high-level thought, they come with a biological trade-off. During early brain development, CUX2 neurons multiply at an exceptionally rapid rate. This speed, however, increases the likelihood of DNA damage accumulating within the cells.
To survive this developmental stress, these cells rely on a specialized “repair kit” driven by a protein called ATF4. This protein jump-starts the DNA repair response, preventing catastrophic damage as the neurons mature. Without ATF4, these cells cannot withstand their own rapid growth and die off.
When the Repair Mechanism Fails
The critical discovery lies in what happens when these already-stressed cells encounter the inflammation of multiple sclerosis.
In healthy brains, the ATF4-mediated repair system keeps DNA damage in check. However, in patients with MS, the chronic inflammation overwhelms this system. The researchers found that:
* Higher DNA Damage: Brain tissue from MS patients showed significantly elevated levels of DNA damage in the layers where CUX2 neurons reside, compared to healthy brains.
* Cellular Collapse: In mice engineered to mimic MS conditions, CUX2 cells died specifically due to this accumulated DNA damage.
* Vulnerability Threshold: The inflammation caused by MS pushes these cells past their breaking point. Because they are already burdened by the risks of their rapid early development, they lack the resilience to handle the additional stress of an autoimmune attack.
“We see this kind of consistent theme that these cells just don’t handle this extra stress very well,” says David Rowitch, a developmental neuroscientist at the University of Cambridge and co-author of the study.
A New Target for Treatment
This finding challenges the traditional focus of MS research. For decades, therapies have primarily aimed at restoring myelin or suppressing the immune system to reduce inflammation. While these approaches help manage symptoms and flare-ups, they do not address the underlying cellular vulnerability that leads to progressive brain atrophy.
“The discovery points to a new place to direct future treatments,” notes Rowitch. Currently, there is no effective treatment for the progressive phase of MS, where neurons die and patients experience sharp declines in memory and reasoning.
Don Mahad, a neurologist at the University of Edinburgh who was not involved in the research, emphasizes the shift in perspective this study requires. “This tells us that actually, we can’t ignore these intrinsic vulnerabilities of the nerve cell, and that has to be a treatment target,” he says.
Conclusion
The identification of CUX2 neuron vulnerability offers a crucial missing link in understanding progressive multiple sclerosis. By recognizing that DNA repair capacity is as critical as immune suppression, scientists can now explore therapies designed to protect these fragile cells from internal damage, potentially halting the cognitive decline that currently defines the later stages of the disease.